Modern Surgical Techniques for Correcting Cleft Lip and Palate
Modern Surgical Techniques for Correcting Cleft Lip and Palate
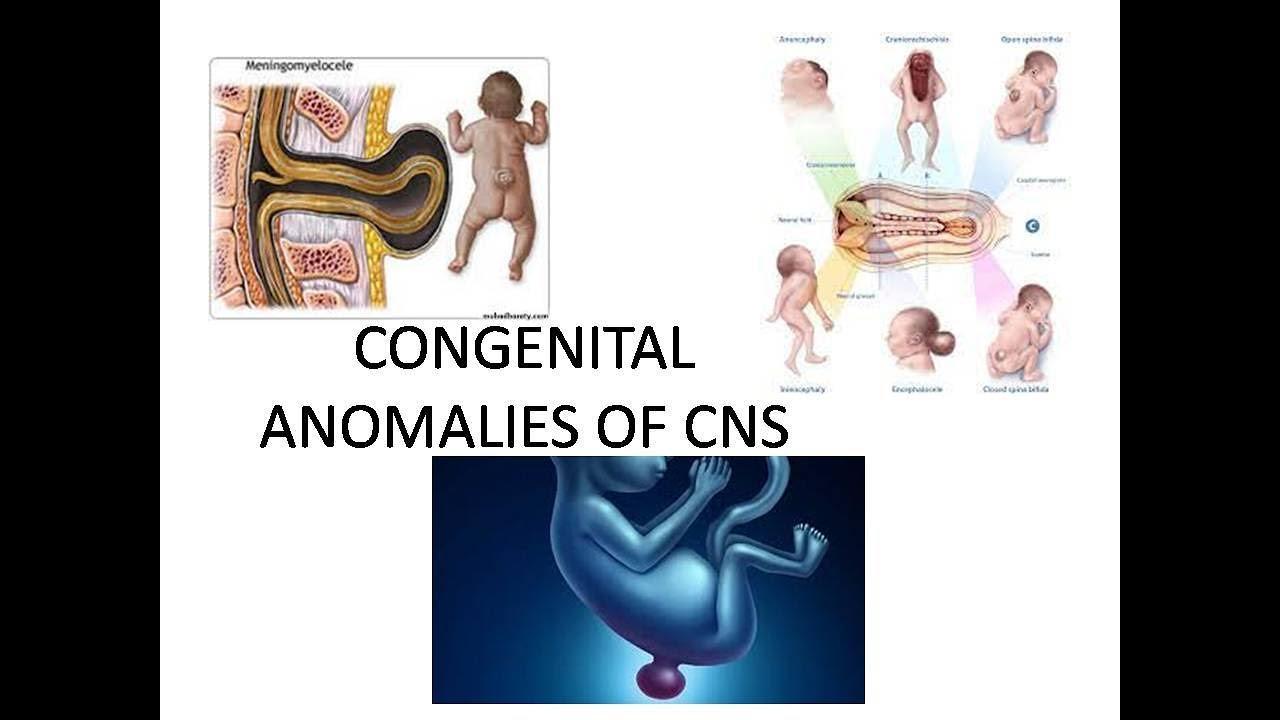
The evolution of pediatric plastic surgery has brought about a new era of precision and hope for families navigating the complexities of facial reconstruction. When addressing Congenital Anomalies in Riyadh, the medical community has placed a significant emphasis on refining the protocols for cleft lip and palate repair, moving beyond simple closure to achieving near-perfect functional and aesthetic restoration. A cleft lip or palate occurs when the tissues of the upper lip or the roof of the mouth do not fuse completely during early fetal development. Today, the approach to treating these conditions is highly sophisticated, involving a carefully timed sequence of interventions that utilize the latest in microsurgical techniques, virtual planning, and bio-compatible materials to ensure that children can breathe, speak, and smile with confidence.
The Philosophy of Early Intervention
Modern surgical philosophy emphasizes the "Rule of Tens" for cleft lip repair, typically performed when an infant is around ten weeks old, weighs ten pounds, and has a stable hemoglobin level. However, the preparation often begins even earlier with Presurgical Nasoalveolar Molding (PNAM). This non-surgical technique involves a custom-made intraoral appliance that gently reshapes the gums, lips, and nostrils before the first surgery. By narrowing the gap in the cleft and improving the symmetry of the nose pre-operatively, surgeons can perform a more tension-free closure, which results in significantly less scarring and a more natural nasal shape.
Advanced Cleft Lip Repair: The Rotation-Advancement Technique
The primary goal of cleft lip surgery is to restore the continuity of the orbicularis oris muscle, which is essential for lip movement and facial expression. The most widely utilized modern technique is the rotation-advancement repair. This procedure involves making precise incisions to "rotate" the displaced tissue into a more natural position and "advancing" the neighboring tissue to fill the gap. Surgeons now use ultra-fine sutures and magnification loupes to meticulously align the "Cupid’s bow" of the lip and the philtrum columns. The focus has shifted from just "closing the hole" to recreating the three-dimensional contours of a natural lip, ensuring that the repair grows harmoniously as the child matures.
Specialized Palatoplasty: Restoring Speech and Function
Cleft palate repair, or palatoplasty, is generally performed between 9 and 18 months of age, a critical window before the child begins to develop significant speech patterns. The modern approach focuses on the "intravellar veloplasty," which involves the meticulous dissection and repositioning of the muscles of the soft palate. By reorienting these muscles into a horizontal, overlapping position, surgeons create a functional "muscle sling" that allows the child to close off the nasal passage during speech and swallowing. This technique has drastically reduced the incidence of velopharyngeal insufficiency (VPI), a condition where air escapes through the nose during speech, resulting in a hypernasal voice.
Alveolar Bone Grafting and 3D Planning
As a child grows, usually between the ages of 8 and 11, many require an alveolar bone graft to fill the gap in the upper jawbone. This is essential for the proper eruption of permanent teeth and the stabilization of the dental arch. Modern advancements in this area include the use of virtual surgical planning (VSP). By using 3D CT scans, surgeons can map out the exact volume of the defect and plan the bone graft with millimeter precision. In some cases, specialized proteins (Bone Morphogenetic Proteins) are used to stimulate the body’s own bone growth, sometimes reducing the need for harvesting bone from the hip, which leads to a faster and less painful recovery for the young patient.
Secondary Refinements and Laser Technology
Even with excellent primary repairs, some children may benefit from secondary refinements as they reach adolescence. These might include tip rhinoplasty to improve nasal symmetry or minor lip revisions. One of the most exciting advancements in post-operative care is the use of fractional CO2 lasers and pulsed-dye lasers. When applied to surgical scars early in the healing process, these lasers can significantly reduce redness and flatten the texture of the scar tissue. This "scar management" protocol is a vital component of the comprehensive care model, ensuring that the physical reminders of the initial anomaly are as faint as possible.
The Multidisciplinary Cleft Team Model
The success of modern surgical techniques is inseparable from the multidisciplinary team approach. A child undergoing cleft repair in a specialized center is managed by a cohesive group that includes:
-
Plastic Surgeons: To perform the intricate reconstructions.
-
Otolaryngologists (ENT): To monitor ear health, as children with cleft palates are prone to fluid buildup in the middle ear.
-
Speech-Language Pathologists: To provide therapy that ensures the surgical repair translates into clear communication.
-
Orthodontists: To manage the alignment of the teeth and jaw over many years.
-
Pediatric Dentists: To maintain specialized oral hygiene.
Psychological Integration and Long-Term Outcomes
The final frontier of cleft care is the psychological well-being of the child. Modern medical sectors have integrated psychologists and social workers into the cleft team to support the child’s self-esteem and social integration. By achieving high-quality surgical results early in life, the "stigma" of a cleft is largely removed, allowing children to enter school and social circles without feeling "different." The ultimate goal of these advanced surgical techniques is to ensure that a congenital diagnosis is merely a brief chapter in a child's life, rather than a defining characteristic, providing them with every opportunity to thrive in a modern world.