Lower GI Endoscopy in the UK: Diagnosis, Procedure, and Patient Care
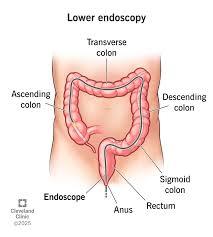
Lower gastrointestinal (GI) endoscopy is an important diagnostic procedure used in the United Kingdom to examine the lower part of the digestive system, including the colon and rectum. It helps doctors identify a wide range of conditions such as bowel cancer, inflammatory bowel disease, polyps, and unexplained abdominal symptoms. In the UK healthcare system, this procedure plays a crucial role in early detection and prevention of serious diseases.
Most lower GI endoscopies are performed through the National Health Service (NHS), ensuring that patients receive timely and accessible care based on medical need. Private healthcare providers also offer the procedure for individuals who prefer faster appointments or additional comfort options.
The most common form of lower GI endoscopy is a colonoscopy. During this procedure, a thin, flexible tube with a camera at the end (called a colonoscope) is inserted through the rectum to examine the lining of the large intestine. This allows doctors to detect abnormalities such as inflammation, bleeding, ulcers, or growths. In some cases, a shorter version called sigmoidoscopy may be used to examine only the lower part of the colon.
Preparation is a key part of the process. Patients are usually required to follow a special diet for a day or two before the procedure and take a bowel-cleansing solution to ensure the colon is completely empty. This preparation is essential for clear visibility during the examination.
The procedure itself typically takes between 20 and 60 minutes. It is usually performed under sedation, which helps patients remain relaxed and comfortable. While mild discomfort or pressure may be felt, most people tolerate the procedure well. During the examination, doctors can also take tissue samples (biopsies) or remove small polyps if necessary. These samples are then sent to a laboratory for further analysis.
Lower GI endoscopy is widely used in the UK as part of bowel cancer screening programs. Early detection of bowel cancer significantly improves treatment success rates, making this procedure a vital tool in public health. It is especially recommended for individuals experiencing symptoms such as persistent abdominal pain, changes in bowel habits, rectal bleeding, or unexplained weight loss.
After the procedure, patients are usually monitored for a short period before being allowed to go home. Because of sedation, they are advised not to drive or operate machinery for at least 24 hours. Mild bloating or gas may occur but typically resolves quickly. Most people can resume normal activities the following day.
Complications from lower GI endoscopy are rare but may include bleeding, infection, or perforation of the bowel. However, these risks are very low, especially when the procedure is performed by experienced specialists. The benefits of early diagnosis and treatment far outweigh the potential risks.
In conclusion, lower GI endoscopy in the UK is a safe, effective, and essential diagnostic procedure that supports early detection and treatment of serious digestive conditions. With advanced medical technology, skilled healthcare professionals, and strong NHS screening programs, patients receive high-quality care that significantly improves long-term health outcomes.